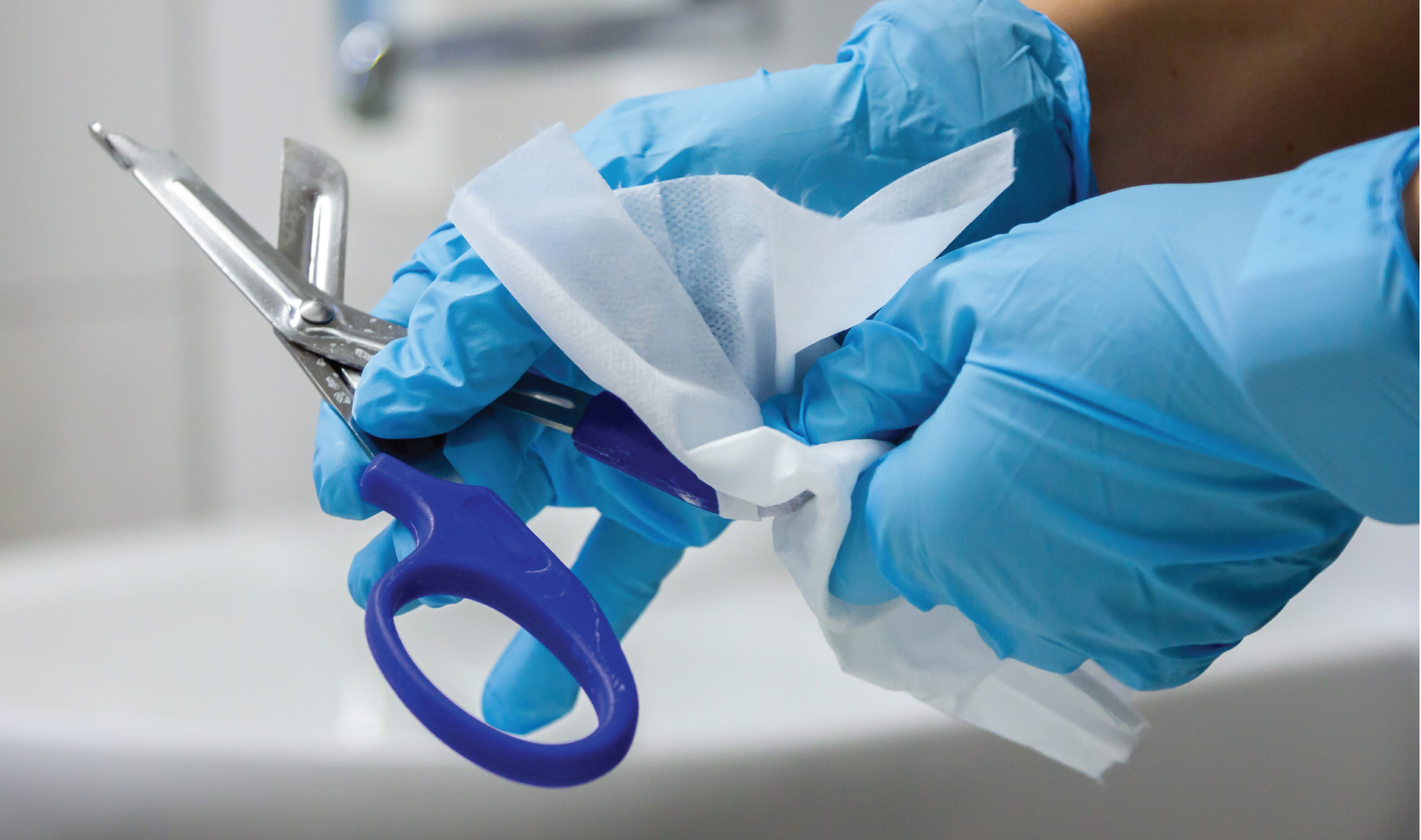
Importance of surface disinfection in dentistry
Dental offices, like other healthcare settings, put patients as well as personnel at risk for healthcare associated infections (HAIs). HAIs are infections that patients can acquire while receiving treatment for another condition in a healthcare setting such as a hospital, dental clinic, outpatient settings (ambulatory surgical centers) or long-term care facility (nursing home, rehabilitation center, etc.)
In dental settings, HAIs are easily transmitted because surfaces such as light handles, switches, X-ray equipment and chair-side computers are touched frequently with gloved hands during patient care or become contaminated with body fluids or other potentially infectious material during dental procedures.
That’s why the CDC recommends that barrier-protected surfaces in dental offices be disinfected at the end of each day or if contamination is evident, and that surfaces that are not barrier-protected be disinfected between patients.1 It is also why, in 2008, the CDC issued its Guideline for Disinfection and Sterilization in Healthcare Facilities.2
Impact of CDC’s Guideline for Disinfectant and Sterilization in Healthcare Facilities
This guideline provided important recommendations for the management of equipment and surfaces in dentistry, including the recommendation in paragraph 8b) that states that “Noncritical clinical contact surfaces, such as uncovered operatory surfaces (e.g., countertops, switches, light handles), should be barrier-protected or disinfected between patients with an intermediate-disinfectant (i.e., EPA-registered hospital disinfectant with a tuberculocidal claim) or low-level disinfectant (i.e., EPA-registered hospital disinfectant with HIV and HBV claim).” 1
Importance of using surface disinfectant correctly
In addition to recommending that operatory surfaces that aren’t barrier protected be disinfected with low-level or intermediate surface disinfectants, the Guideline also emphasized the importance of using the selected surface disinfectant correctly. To drive home the importance of following product label instructions, the CDC went as far as to make it a legal obligation.
Paragraph 5k) of the same guideline stipulates that “by law, the user must follow all applicable label instructions on EPA-registered products. If the user selects exposure conditions that differ from those on the EPA-registered product label, the user assumes liability for any injuries resulting from off-label use and is potentially subject to enforcement action under FIFRA.”
| Example |
|---|
| If a hygienist or dentist uses a disinfectant with a 10-minute contact time and does not let the disinfectant remain wet on the surface for the full 10 minutes, he or she assumes liability for any infections transmitted. |
Once users became legally responsible for using surface disinfectants correctly, dental and other medical offices stopped using approximately 80% of the surface disinfection products they’d been using whose contact time was too long to be practically followed. To meet their legal obligations without compromising their efficiency, they began seeking disinfectants with a contact time of no longer than 1 minute.
Understanding “Contact Time”
The CDC defines contact time as the time a disinfectant is in direct contact with the surface or item to be disinfected. For surface disinfection, this period is framed by the application to the surface until complete drying has occurred. In other words, it refers to how long a disinfectant must remain wet on a surface to effectively eliminate all the pathogens listed on its label. Products with long contact times can evaporate before effectively disinfecting the surface, particularly when used in high temperature/low humidity environments. This means that successful disinfection would require multiple reapplications of the product, resulting in wasted time and money.
Products with long contact times also reduce compliance because it’s harder to use them correctly. Few dental office team members have the time—or the desire—to stand around to make sure the disinfectant product they’re using remains wet for up to 10 minutes or more.
Another problem with surface disinfectants is that many users are in the habit of immediately rinsing or wiping the surface dry after applying the product when, achieving successful disinfection requires that they wait the required contact time listed on the label before drying or rinsing. That’s why it’s so important to choose a surface disinfectant with a short contact time to achieve disinfection quickly against fungicidal, bactericidal and virucidal pathogens.
Other factors to consider
In addition to a short contact time, there are several other factors to consider when choosing a surface disinfectant. Reading the product label will allow you to consider the following four selection criteria:
empty title
- Kill Claims
- Kill Times
- Product Safety
- Ease of Use
empty title
- Does the product kill the pathogens that are of concern in your facility? Remember to consider both Healthcare Associated Infections (HIAs) and those that can cause outbreaks/pandemics.
- Whereas “contact time” is the time it takes a disinfectant to kill all the pathogens listed on its label, “kill time” is the time it takes a disinfectant to kill an individual pathogen/group of pathogens. This is an important factor to consider, particularly if specific pathogens are of concern in your area.
- Does the product have acceptable toxicity and flammability ratings? Is it compatible with most surfaces in your facility? Is personal protection equipment required when using it?
- Is the product ready to use or does it require preparation? Does the product come in convenient formats like wipes and spray? Does it clean and disinfect in a single step, or are multiple steps required?
When all surface disinfectant selection criteria are considered, Medicom ProSurface disinfectant wipes and spray are the obvious choice for your practice.
Medicom ProSurface disinfectant wipes and spray
In addition to having a short 60-second contact time and being effective against Human Coronavirus, Medicom ProSurface wipes and spray with TotalClean™ technology eliminate 48 pathogens, including bacteria, fungi, TB and viruses, without damaging surfaces and with little to no residue.
| While a short contact time is always beneficial, it’s even more important now, as the pandemic lingers. By choosing a product like Medicom ProSurface that is effective against the coronavirus and has a short contact time, you and your staff can spend less time disinfecting and more time treating your patients. |
|---|
| ProSurface kills all pathogens listed on the label in just 1 minute. Therefore, it has a 1-minute contact time and only needs to remain wet on a surface for 1 minute to be fully effective. |
ProSurface is an intermediate level disinfectant that disinfects and deodorizes non-critical environmental and non-porous hard surfaces and inanimate objects. It requires no special handling and meets CDC guidelines for disinfection in healthcare facilities, as well as all US EPA and Health Canada requirements.
ProSurface has been tested on a wide variety of hard surfaces commonly found in dental settings, such as granite countertops, plastic backing and covers, various metal dental chair parts, keyboard covers and more.
ProSurface is effective against Human Coronavirus
Since 1988, Medicom has actively worked to supply our customers with protective products through major health crises such as HIV, SARS and the Ebola outbreak. Medicom ProSurface disinfectant line has a 1-minute kill claim for Human Coronavirus.

ProSurface disinfectant wipes are ideal for use between patients, while ProSurface disinfectant spray gets into smaller cracks and crevices for even more thorough end of day cleaning. For best results, use ProSurface spray with ProSurface dry wipes. Made in the USA from top quality cellulosic and synthetic fibres, ProSurface non-woven dry wipes offer exceptional absorbency and tear resistance and are suitable for deep cleaning of large non-porous surfaces.
To learn more about Medicom disinfectant products, please visit our website.
Footnotes
- Centers for Disease Control and Prevention. Guidelines for Infection Control in Dental Health-Care Settings — 2003. MMWR 2003;52(No. RR-17):26.
- Guideline for Disinfection and Sterilization in Healthcare Facilities, 2008, William A. Rutala, Ph.D., M.P.H., David J. Weber, M.D., M.P.H. and the Healthcare Infection Control Practices Advisory Committee (HICPAC); Updated 2019 https://www.cdc.gov/infectioncontrol/guidelines/disinfection/index.html; Accessed Nov.5, 2021.



 English (US)
English (US)